Variation in Prostaglandin Analog Prices Analyzed
Providers don’t usually ask what type of Medicare Part D plan their patients with glaucoma have but it’s something that should be considered, according to Aaron Priluck, BSE, of the Department of Ophthalmology and Visual Sciences at the Truhlsen Eye Institute in Omaha, NE, who recently analyzed the price variation of prostaglandin analogs (PGAs). Discussing whether it makes sense to change supplemental plan coverage during the next enrollment period should also be a topic of conversation, he urged.
Remember, however, that there are a number of moving parts to consider.
Using 2013-2015 Medicare Part D prescriber data, Priluck and colleagues calculated the city, state, and national standard deviations and ranges of prices for these seven PGAs: bimatoprost, latanoprost, Lumigan, Travetan Z, travoprost, Xalatan, and Zioptan. They also looked at whether price was affected by income and population. Additionally, they calculated the savings if the same PGA was purchased in the same city at the lowest price found in that city.
A Significant Issue
The issue is significant because glaucoma costs Medicare Part D more than any other eye condition, comprising $1.4 billion of a $2.9 billion total in 2015, explained Priluck. PGAs made up $765 million of the total. He cited data showing that approximately 40% of glaucoma patients experience difficulty paying for their glaucoma medications, and may not be getting the lowest price [Patient-reported behavior and problems in using glaucoma medications. Ophthalmology. 2006; 113(3):431-436].
Priluck found that, with the exception of latanoprost, average prices for the analyzed PGAs ranged from $100 and $140 for a 30-day supply, ticking upward slightly each year. Meanwhile, latanoprost was <$20/month and trending slightly downward. Moreover, the intracity range “is actually staggering. In some cases, the range is more than the prices of the drugs themselves,” said Priluck (see accompanying table).
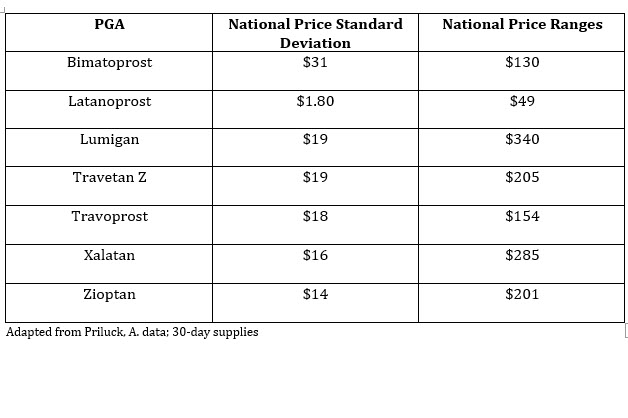
“When looking at…all drugs except for latanoprost, the intracity standard deviation in price is about $10 to $20.” He extrapolated that “16% of our patients are paying $10 or more per month for the same PGA that their counterparts in the same city are paying less for.”
Prices did not strongly correlate to income or population, leaving researchers to surmise that plan choice impacted what patients pay. “There is substantial variation in the price at the provider level,” explained Priluck. “More variation likely exists at the patient level. There is no indication that the variation is decreasing, so this is not a problem that will solve itself.”
The difference can add up. In fact, Priluck and colleagues estimate that “$122 million would have been saved in 2015 if each PGA was purchased at the lowest intracity price.”
Many Moving Parts
Of course, the matter is not that straightforward when considering other factors. Not all plans are available to everyone, and the distribution of savings is unclear, he said. Most important, “patients should not optimize their plan based solely on PGAs, since most of these patients are taking other medications.”
Additionally, although Priluck’s study did not analyze pharmacy choice, patients can also optimize their pharmacy to get the best price. But while a plan or pharmacy change might result in saving money on a PGA, if the drug needs to be purchased across town, poor adherence might come into play if getting to that pharmacy is inconvenient. It is also important to note that if you have a patient who is noncompliant due to cost, it might be worth considering a mail order service that delivers both potential cost-savings and convenience.
The bottom line: There are many moving parts.
Still, it is not a bad idea to raise the issue of plan choice with patients via support staff or patient education materials. Data shows that 87% of Medicare recipients do not switch their plan during open enrollment [Hoadley J, Hargrave RE, Summer L, Cubanski J, Neuman T. To switch or not to switch: Are Medicare beneficiaries switching drug plans to save money? Kaiser Family Foundation. 2013]. Moreover, a study found that optimizing plan choice considering all drugs taken can results in a nearly $1,200 annual savings per patient [Leonard C, Cohenour F, DeLoach L, Galdo J. Impact of an open enrollment service on costs for Medicare Part D beneficiaries. J Am Pharm Assoc (2003). 2017;57(3S): S225-S228].
The open enrollment period for 2020 will be October 15 through December 7, 2019.
Finally, Priluck pointed out what many already know: Prescribing generics reduces costs. Unless clinicians are considering one of the newly-approved glaucoma medications for their effect (such as BAK-free latanoprost or latanoprostene bunod, which we covered recently), going with a generic will undoubtedly save money. “In 2015, prescribing generic latanoprost, bimatoprost, or travoprost would have saved about 90%, 30%, and 35% off the costs of those brand name drugs, respectively.”
The PGAs analyzed in Priluck’s study “are all the same,” noted Wiley Chambers, MD, a supervisory medical officer at the FDA. “The reason most ophthalmologists in this country have difficulty with generic products is that they don’t understand which products are generics and which are not. Just because a product has the same established name as a generic does not make it a generic.”
Refernce
Priluck A, Havens S. Intra-city, intra-state, and national variation in prostaglandin analogue prices. Talk presented at: AAO 2018 annual meeting; October, 26-30, 2018; Chicago.